What is a viability scan? A viability scan is a medical test that can be used to assess the health of the developing fetus in utero. It involves using ultrasound to determine if there are any signs that the baby may need emergency, or non-urgent, intervention. If an abnormality is found, it can cause an increase in fetal distress and it will be necessary for a more invasive procedure to be performed on the baby. Can I do an early fetal viability scan at home? Yes, you can purchase a home pregnancy test kit and perform your own early fetal viability scans at home. These kits generally have a window where you can do a scan..
Understanding the Different Types of Foetal Viability Scans in India
Oxygen delivery systems are essential for providing adequate oxygen supply to infants and pregnant women. Continuous positive airway pressure (CPAP), biphasic positive airway pressure (BiPAP) and nasal cannula oxygen delivery systems are the three most commonly used types of oxygen delivery systems in the medical field. CPAP is used to treat sleep apnea, BiPAP is used for those with more severe sleep apnea, and nasal cannula oxygen delivery system is often used for infants and pregnant women who require additional oxygen support. Each has its own unique benefits and drawbacks, so it is important to understand the differences between them in order to determine which one is best suited for a particular patient's needs.
What Are the Best Practices for Administering Supplemental Oxygen Therapy to Infants & Pregnant Women?
Fetal viability scans are an important part of pregnancy care in India. These scans help to monitor the development of the fetus, identify any potential risks and ensure that the mother and baby remain healthy throughout the pregnancy. There are three different types of fetal viability scans available in India – first trimester viability scan, second trimester ultrasound scan and 3d/4d ultrasound scan. Each type of scan
First trimester viability scan- A first trimester viability scan is a screening examination performed in the first 12 weeks of pregnancy. This test involves an ultrasound scan to evaluate the size and development of the fetus, as well as an assessment of maternal blood levels, including workup for protein levels in case there is a risk to the health of either mother or her unborn child. First trimester scans are commonly requested by women who are pregnant for the first time, or those with multiple pregnancies. The main goal of a first trimester viability scan is to identify any potential risks that could complicate the pregnancies, so that appropriate treatment can be given. First trimester scans are typically performed between 12 and 15 weeks of gestation, in order to allow time for any potential complications to manifest themselves before continuing the pregnancy. The scan is scheduled to coincide with the mother's next period, so that the pregnancy can be monitored after it has reached full term. The accuracy of first trimester viability tests is dependent on gestational age and maternal blood markers being measured accurately. It should also be noted that inaccuracies in a first trimester viability test are not an indication of a miscarriage, although they may appear as such when they are not present. Ultrasound scans play an integral role in this examination but do have limitations as well. There are risks involved with undergoing such tests which include infection, complications from anesthesia , and fetal anomalies. Ultrasound scans are conducted in order to provide a detailed image of the fetus, which is critical for monitoring the pregnancy. The scan provides an image of the fetus from the face down to its lower limbs, using sound waves to provide an estimate of its size and mass.
Benefits of a Foetal Viability Scan and How to Prepare for One
Fetal viability scans are essential for the health of both mother and baby. They provide valuable information about the development of the fetus, enabling medical professionals to identify any potential issues early on. It is important for expectant mothers to be aware of the benefits of a fetal viability scan and how to prepare for one. A fetal viability scan can help detect any abnormalities in the development of the fetus, such as structural defects or genetic disorders. It can also help determine if there is sufficient amniotic fluid around the baby, which is essential for its growth and development. Furthermore, it can provide an estimate of when delivery will take place, allowing medical professionals to plan accordingly. Preparing for a fetal viability scan involves scheduling an appointment with a maternal care doctor in India and getting a full health checkup report done prior to the scan. Additionally, it is important to ensure that you are well rested before attending your appointment so that you are relaxed and in a good mood. The best time to attend your scan is between the weeks of 8 and 14 weeks of pregnancy. A fetal viability scan is a non-invasive, painless test that uses imaging techniques such as ultrasound or Doppler to detect any abnormalities in the development of the baby. A fetal viability scan involves taking images from different angles including transverse, sagittal, and fetal head views with a vaginal probe. Ultrasound also detects amniotic fluid levels as well as size and gestational age of the infant. While a baby's gestation age can be determined by measuring the length of its head, an amniocentesis is sometimes needed to accurately determine this age.The following are some of the ways a fetal viability scan can detect abnormalities:In most cases, a doctor or nurse practitioner will run through any anomalies they may see on the screen during your appointment.
What Is Supplemental Oxygen Therapy And How Does It Help With Infant And Pregnancy Health?

Dec 05, 2023 | 6 comments Reference
Supplemental oxygen therapy
Supplemental oxygen therapy is a medical treatment used to provide additional oxygen to people who need it due to medical conditions, such as low blood oxygen levels. It is often used for infants and pregnant women, as well as people with chronic respiratory problems. Oxygen therapy helps these individuals breathe easier and more comfortably, and can even help improve their overall health. In this article, we will discuss how supplemental oxygen therapy works, the risks associated with it, and how it can be beneficial for infants and pregnant women. Oxygen therapy helps people breathe more easily and comfortably.
Oxygen Therapy: How It Works When a person has low oxygen levels in their blood, supplemental oxygen can be delivered to their lungs via a non-rebreathing mask. The mask will absorb the carbon dioxide build up, while releasing clean oxygen into the patient's lungs. In some cases, this may also help with other problems such as chest pain or headache. Oxygen therapy is often used for babies and pregnant women because it can reduce the risk of complications from low oxygen levels during these critical times in their lives. For people with chronic lung diseases such as COPD, oxygen therapy can help alleviate shortness of breath.
Understanding the Different Types of Oxygen Delivery Systems Used During Infant & Pregnancy Care
Oxygen delivery systems are essential for providing adequate oxygen supply to infants and pregnant women. Continuous positive airway pressure (CPAP), biphasic positive airway pressure (BiPAP) and nasal cannula oxygen delivery systems are the three most commonly used types of oxygen delivery systems in the medical field. CPAP is used to treat sleep apnea, BiPAP is used for those with more severe sleep apnea, and nasal cannula oxygen delivery system is often used for infants and pregnant women who require additional oxygen support. Each has its own unique benefits and drawbacks, so it is important to understand the differences between them in order to determine which one is best suited for a particular patient's needs.
CPAP uses a mask to deliver pressurized oxygen to patients with sleep apnea. It is an effective treatment for obstructive sleep apnea, which is when the airway becomes obstructed by excessive tissue in the throat and nose. The device blows air into the patient's lower respiratory tract to keep their airway open and allows them to breathe properly. CPAP can also be used as a treatment for moderate sleep apnea, but it will not work on those with chronic or severe symptoms without further evaluation of their condition by a specialist. CPAP can cause problems with breathing while sleeping because it presses against the soft tissue in the mouth and nose while mask straps apply pressure to the head.
Supplemental oxygen should be discontinued after delivery because rates at which infants are exposed to high-level O 2 can be harmful to the baby. The most common method of supplemental oxygen therapy is nasal cannula; however, it can also be supplied by a face mask or a continuous positive airway pressure (CPAP) machine. If the woman is able to tolerate using these machines, they may be more appropriate than nasal cannulas. In some cases, an oral or facial mask may need to be used because there is an inability or difficulty in using the CPAP machine or the woman cannot tolerate it.
What Are the Best Practices for Administering Supplemental Oxygen Therapy to Infants & Pregnant Women?
Administering supplemental oxygen therapy to infants and pregnant women can be a challenging task. It is important to understand the best practices for administering oxygen therapy in order to ensure the best outcomes for patients. Neonatal hypoxemia treatment guidelines should be followed when providing oxygen therapy, as well as proper administration of high flow nasal cannula. Additionally, care should be taken to ensure that oxygen levels are monitored closely and that appropriate adjustments are made if needed. By following these best practices, medical professionals can provide safe and effective supplemental oxygen therapy for infants and pregnant women.
Best Practice for Supplemental Oxygen Therapy It is important to use a standard face mask or nasal cannula during oxygen therapy. It is recommended that supplemental oxygen be delivered via a non-rebreathing face mask. The standard face mask delivers only the patient’s inspired air and exhalation, while the non-rebreathing mask delivers both the patient’s inspired and expired air. If a non-rebreathing mask is unavailable, it can be used in conjunction with a nasal cannula with high flow settings as long as it does not impede breathing.
The Importance of a Well-Informed Patient in Discussing Supplemental Oxygen Therapy
Supplemental oxygen therapy is a life-saving treatment that can prevent the progression of respiratory failure and improve the quality of life for many patients. In order to provide optimal supplemental oxygen therapy, it is important that patient education is tailored to their individual needs. By understanding the risks, benefits, and potential side effects associated with supplemental oxygen therapy, patients can make informed decisions about whether or not they wish to receive it.
Patient education is an important factor in providing successful supplemental oxygen therapy. It is essential for a patient to be well-informed about their condition and treatment plan in order to have effective communication with their healthcare provider and ensure continuity of care. By understanding the risks, benefits, and potential side effects associated with supplemental oxygen therapy, patients can make informed decisions that are tailored to their individual needs. This article will discuss the importance of a well-informed patient when discussing supplemental oxygen therapy and how it can help promote better outcomes.
Understanding Acute Respiratory Distress Syndrome (ARDS) in Infants and During Pregnancy
Oct 26, 2023 | 9 comments Reference
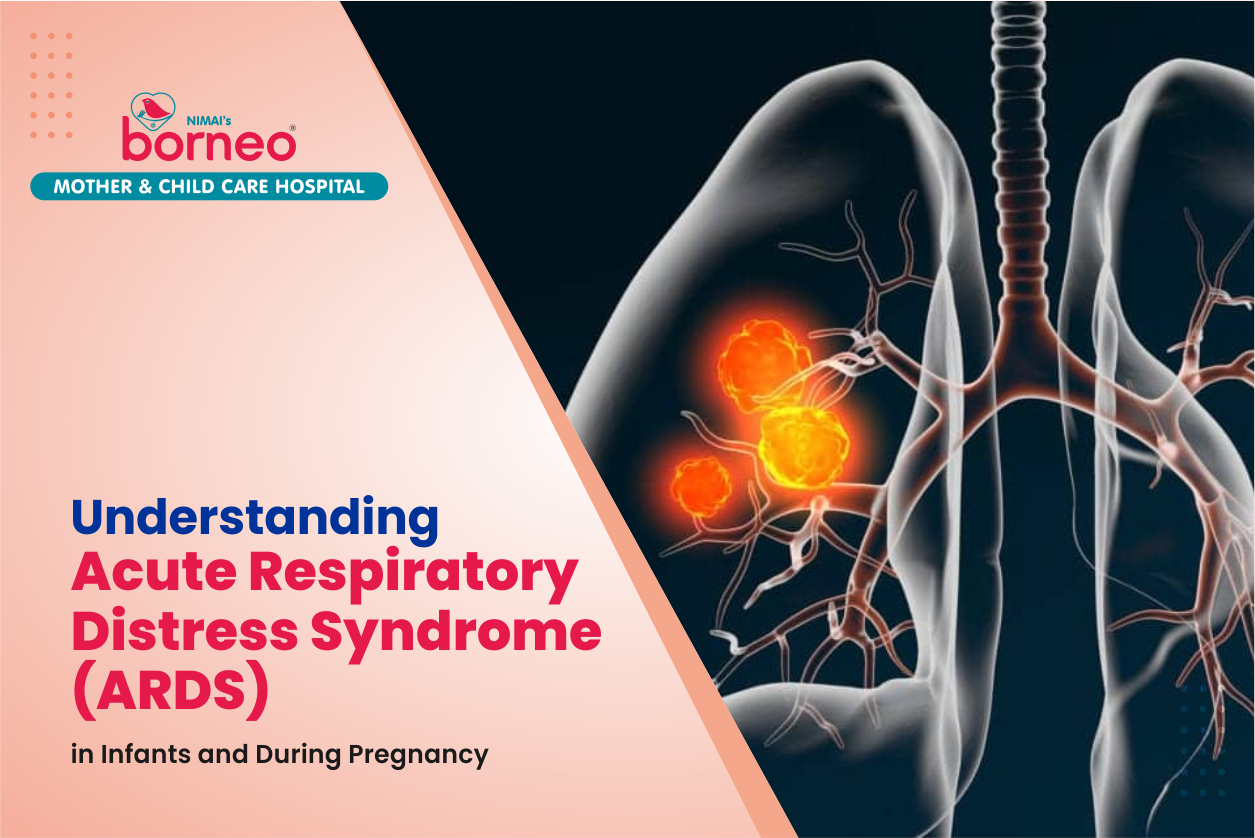
Introduction: What is ARDS and How Does It Affect Infants and Pregnant Women?
Acute respiratory distress syndrome (ARDS) is a severe form of lung injury that can lead to life-threatening breathing difficulties. It is a medical emergency and requires immediate treatment.
There are many potential causes of FGR, including maternal malnutrition, smoking, alcohol consumption or drug use during pregnancy. Awareness of these risk factors is essential in order to identify and manage the condition appropriately. Early diagnosis and treatment are key to ensuring the best possible outcome for both mother and baby. It is important for medical professionals to be aware of the signs and symptoms of FGR so that they can diagnose it quickly and provide appropriate care. This includes monitoring fetal growth patterns throughout pregnancy as well as providing nutritional support to mothers with risk factors such as malnutrition or substance abuse during pregnancy.
Signs and Symptoms of ARDS in Infants and Expectant Mothers
Acute Respiratory Distress Syndrome (ARDS) is a life-threatening condition that affects infants and expectant mothers. It is caused by a severe infection in the lungs which can lead to difficulty in breathing and oxygen deprivation. Some of the common symptoms of ARDS include rapid breathing, shortness of breath, grunting sounds while breathing, and low oxygen levels. In some cases, the infant may have bluish skin due to lack of oxygen.
Preeclampsia is another condition that can be related to ARDS and is characterized by high blood pressure during pregnancy. Symptoms of preeclampsia include swelling in the hands and face, headaches, vision changes, nausea or vomiting, sudden weight gain or loss, and abdominal pain.
If you suspect that your infant or expectant mother has ARDS or preeclampsia it is important to seek medical attention immediately as it can be fatal if not treated promptly. Treatment for ARDS typically involves providing supplemental oxygen while treatment.
The Common Symptoms & Diagnostic Tests for ARDS
Acute Respiratory Distress Syndrome (ARDS) is a life-threatening condition that affects the lungs. It occurs when fluid builds up in the air sacs of the lungs, making it difficult for oxygen to get into the bloodstream. The common symptoms of ARDS include difficulty breathing, rapid breathing, and low blood oxygen levels. Diagnostic tests such as chest x-rays, pulmonary function tests, and blood tests are used to diagnose ARDS. In this article, we will discuss the common symptoms and diagnostic tests for ARDS.
Diagnosis of ARDS in Infants & Pregnant Mothers
Early diagnosis of ARDS is essential to ensure timely treatment and improve the chances of recovery. In infants, the diagnosis of ARDS involves assessing symptoms such as rapid breathing, labored breathing, and poor oxygen levels in the blood. For pregnant mothers, preeclampsia is one of the main risk factors for developing ARDS and should be monitored closely during pregnancy. Diagnosis of preeclampsia includes checking for high blood pressure, proteinuria, and edema. Treatment for both conditions includes providing supplemental oxygen, mechanical ventilation if needed, antibiotics to treat any underlying infections, and medications to reduce inflammation.
Treatment Options for ARDS Patients
Acute Respiratory Distress Syndrome (ARDS) is a life-threatening condition that affects the lungs and can be caused by a variety of conditions, including pneumonia, sepsis, and trauma. Treatment options for ARDS patients vary depending on the cause and severity of the condition. For infants, treatment often involves providing oxygen to help them breathe easier, as well as medications to reduce inflammation in the lungs and prevent further damage. Preeclampsia is another condition that can lead to ARDS during pregnancy; treatment options for this include medications to control blood pressure and reduce fluid buildup in the mother's body. In some cases, delivery may be recommended if the risk of complications is too high.
Preeclampsia is a condition that affects the blood pressure, fluid build-up, and protein in a pregnant woman. It can cause preeclampsia symptoms such as high blood pressure and swelling in the hands, feet, or face. Preeclampsia can lead to serious health complications, including premature birth and eclampsia. Treatment options for this condition may include medications to control blood pressure (Lamictal), prevent organ injury (aspirin), reduce fluid buildup by controlling nausea and vomiting (reglan), or use of magnesium sulfate to balance out abnormal proteins in the blood.
Caring For an ARDS Patient
Caring for a preterm infant with respiratory distress syndrome (ARDS) can be a challenge for both the infant and the mother. It is important to provide proper care and treatment to ensure that the infant recovers quickly and without any complications. In addition, it is also important to take care of the mother who may be suffering from preeclampsia. This article will discuss some of the key steps involved in caring for an ARDS patient, including proper nutrition, monitoring oxygen levels, administering medications, and providing emotional support. Additionally, it will discuss how to provide care for a mother with preeclampsia so that she can receive adequate rest and nutrition while caring for her infant.
How to Improve Outcome & Reduce Complications with ARD
Acute respiratory distress syndrome (ARDS) is a life-threatening condition that affects the lungs and can lead to severe complications. To improve the outcome and reduce complications associated with ARDS, it is important to focus on nutrition, physical activity, and other therapeutic interventions. Nutrition plays an important role in helping ARDS patients recover. Proper nutrition helps to reduce inflammation and improve the patient's overall health. Physical activity is also essential for ARDS patients as it helps them build strength and endurance while in the ICU. Other therapeutic interventions such as breathing exercises can also help in improving outcomes and reducing complications associated with ARDS. With proper care, ARDS patients can make a full recovery from their condition.
The Dangers of Fetal Growth Restriction
Oct 26, 2023 | 14 comments Reference
Introduction: What is Fetal Growth Restriction (FGR) & What Are The Causes?
Fetal Growth Restriction (FGR) is a condition in which the fetus does not grow as expected during pregnancy. It is also known as Foetal Intrauterine Growth Restriction (IUGR). FGR can result in serious health complications for both the mother and baby, and can even be fatal. It is important to understand the causes of FGR so that it can be identified early and managed appropriately.
There are many potential causes of FGR, including maternal malnutrition, smoking, alcohol consumption or drug use during pregnancy. Awareness of these risk factors is essential in order to identify and manage the condition appropriately. Early diagnosis and treatment are key to ensuring the best possible outcome for both mother and baby. It is important for medical professionals to be aware of the signs and symptoms of FGR so that they can diagnose it quickly and provide appropriate care. This includes monitoring fetal growth patterns throughout pregnancy as well as providing nutritional support to mothers with risk factors such as malnutrition or substance abuse during pregnancy.
What is IUGR?
Intrauterine growth restriction is defined as a decrease in foetal growth from the established norm. This might include a decrease in head circumference, weight, or other measures. The problem is usually detected by measuring body length and head circumference of the fetus during the second trimester of pregnancy. Intrauterine growth restriction typically occurs when an individual's weight gain falls below what is considered normal for their height. If this happens every month, it can be seen as "normal" even though it may be outside the healthy range for that particular individual. The most common cause of IUGR is maternal diabetes, and an increased risk of fetal growth restriction exists with maternal diabetes, preeclampsia, renal disease, and other chronic diseases such as hepatitis. Another cause is placental insufficiency.
Understanding How Fetal Growth Restriction can Lead to Serious Complications-
It is important to diagnose FGR early in pregnancy as it can lead to serious complications. The size of the fetus can be monitored during antenatal care, and if there is any concern about FGR, further tests should be done to diagnose it. FGR can lead to premature birth and low birth weight, which can increase the risk of health problems for both mother and baby. It is, therefore, important for pregnant women to seek regular antenatal care so that any issues with fetal growth can be detected early on and managed appropriately.
How to Choose a Quality and Affordable 4D Scan Service Provider
Choosing the right 4D scan service provider can be a tricky task. With so many options out there, it's important to find one that offers quality scans at an affordable price. Fortunately, there are a few tips and tricks you can use to make sure you get the best 4D scanning services available. When selecting a 4D scan service provider, look for one that has experience in providing prenatal care clinic services. Also, make sure they offer 3-4-dimensional scans with the latest technology and equipment.
Additionally, check their customer reviews and ratings to ensure they have a good reputation in the industry. Finally, compare prices from different providers to find an affordable option that meets your needs and budget. When taking a 4D scan, it's important to do your research and find a provider that offers quality images at an affordable price. Using these tips and tricks will help you narrow down the options and make the best decision possible.
How to Reduce the Risks of a 4D Scan by Conducting Simple Maintenance and Avoiding Unnecessary Procedures?
During pregnancy, it is important to reduce the risks associated with a 4D scan by conducting regular maintenance and avoiding unnecessary procedures. A 4D scan is a type of ultrasound that provides detailed images of the baby's development in the womb. While this technology can be incredibly beneficial for expectant parents, it also comes with certain risks. By conducting simple maintenance and avoiding unnecessary procedures, you can reduce these risks and ensure your baby's safety during this important time.
Maintain your weight gain throughout pregnancy: Maintaining a healthy weight gain is one of the most important steps in reducing pregnancy risks. If you are struggling to meet your weight gain goals, talk to your doctor about talking with them about dietary changes and other possible solutions that can make it easier on you and the baby. Discuss what you should be eating each day, how much, and when in order to make sure that this process is going as smoothly as possible for both you and the baby.
Go for an ultrasound every six weeks: Getting your regular ultrasound is an easy way to monitor how your baby is developing. This will also give you peace of mind that everything is running smoothly and any problems you may be having, whether it be with the placenta or the baby, will be caught before they progress too far.
The third phase is postnatal care with a focus on providing physical support to breastfeeding mothers as well as emotional support to new mothers who are experiencing postpartum depression or other mental health challenges.
Discuss your anxiety with a doctor: Anxiety can make pregnancy and motherhood difficult for some women and while it can't always be prevented, a lot of doctors in the field believe that one reason for this anxiety stems from poor symptom recognition and poor communication between patients and their doctors. This means that there are many things you could be doing that you are not aware of, and once pinpointed, will make a big difference.
What are Different Types of Equipment Used in a 4D Scan?
4D scans are the latest developments in fetal imaging technology, allowing expecting parents to get a detailed view of their baby’s development. 4D scans use specialized equipment to capture three-dimensional images of the fetus in real time. This provides a more accurate picture of the baby’s size, shape, and movements than traditional 2D scans. To perform a 4D scan, medical professionals must use specific types of equipment such as ultrasound machines, fetal monitors, and 3-4-dimensional scanners. With this technology, parents can get an up close look at their unborn child and gain insight into their development before birth.
A Holistic Approach to Keeping Your Baby Healthy

Sep 18, 2023 | 13 comments Reference
All You Need Is Love & Lamaze – The Benefits of Lamaze During Childbirth
Lamaze therapy is an evidence-based holistic approach to pregnancy and fetal care that helps to keep the baby healthy. It is a natural childbirth method that promotes active participation of the mother during labor and delivery. It involves breathing techniques, relaxation, massage, and other activities that help to reduce pain and anxiety during labor.
Lamaze therapy also helps to promote better communication between the mother and her healthcare provider. This approach also provides education on pregnancy health, nutrition, exercise, labor positions, birth plans, and postpartum care. By using a holistic approach such as Lamaze therapy for pregnancy and fetal care, mothers can ensure that their babies are born healthy and happy.
Lamaze Therapy for Pregnancy

Oct 09, 2023 | 5 comments
What is Lamaze Therapy and How Does it Help During Pregnancy?
Lamaze therapy is a type of prenatal care that focuses on providing expectant mothers with the knowledge, skills, and support they need to have a healthy pregnancy and childbirth experience. It is based on the belief that childbirth is a natural process that should be experienced with minimal medical intervention. Lamaze therapy teaches expectant mothers about their bodies and how to use breathing techniques, relaxation exercises, massage, and other comfort measures during labor and delivery. In addition to helping women cope with pain during childbirth, Lamaze therapy also helps them understand their options for labor and delivery so they can make informed decisions about their care.
Benefits of Practicing Lamaze Therapy During Pregnancy
Practicing Lamaze therapy during pregnancy can provide a variety of benefits for expecting mothers. Lamaze therapy is a type of prenatal exercise and breathing technique that helps pregnant women prepare for labor and delivery.
Pregnant women may attend childbirth education classes, prenatal exercise and breathing training, or Lamaze training to prepare for labor.
These types of prenatal exercises are typically taught in a group setting with an experienced childbirth educator or instructor. In some facilities (such as hospitals), pregnant women are given individualized instruction from a trained professional in preparation for labor and delivery.
What is Lamaze Therapy and How Does it Help During Pregnancy?
Lamaze therapy is a type of prenatal care that focuses on providing expectant mothers with the knowledge, skills, and support they need to have a healthy pregnancy and childbirth experience. It is based on the belief that childbirth is a natural process that should be experienced with minimal medical intervention.
Lamaze therapy teaches expectant mothers about their bodies and how to use breathing techniques, relaxation exercises, massage, and other comfort measures during labor and delivery. In addition to helping women cope with pain during childbirth, Lamaze therapy also helps them understand their options for labor and delivery so they can make informed decisions about their care.
Benefits of Practicing Lamaze Therapy During Pregnancy
Practicing Lamaze therapy during pregnancy can provide a variety of benefits for expecting mothers. Lamaze therapy is a type of prenatal exercise and breathing technique that helps pregnant women prepare for labor and delivery.
It also provides strategies for labor coping, such as relaxation, distraction, and positioning.
Practicing Lamaze therapy during pregnancy can help reduce pain during labor, speed up delivery time, and promote overall physical and mental wellbeing.
It can help reduce stress levels in both the mother and baby before birth, which is beneficial for both the mother and baby.
It can be a very calm and relaxing experience for both the mother and the newborn,
Pregnant women may attend childbirth education classes, prenatal exercise and breathing training, or Lamaze training to prepare for labor. These types of prenatal exercises are typically taught in a group setting with an experienced childbirth educator or instructor. In some facilities (such as hospitals), pregnant women are given individualized instruction from a trained professional in preparation for labor and delivery.
Exploring Different Types of Lamaze Exercises and Positions That Can Be Used During Labour
Lamaze exercises are an important part of pregnancy and labor. They help to prepare the body and mind for the physical and emotional changes that can occur during labor. Stretching exercises, pelvic floor exercises, and relaxation techniques are all important components of Lamaze exercises. These can be used to increase flexibility, strength, and comfort during labor. Different types of Lamaze exercises and positions can be used during labor to ensure a safe delivery. We will also discuss how these exercises can help with pain management during labor.
Tai chi is a traditional Chinese martial art that can be traced back to the 13th century. It is also widely practiced today in many cultures, including North America and Europe. This form of movement incorporates slow, smooth, flowing movements to promote wellbeing and balance. Tai chi is often practiced as an integrative therapy for achieving relaxation and physical fitness.
Some other forms of Lamaze exercises that are often used during labor are yoga poses and breathing techniques. These can be combined with walking or bicycling to increase endurance levels during labor.
The Role of a Certified educators in Pregnancy Care and Delivery
The Role of a Certified educators in Pregnancy Care and Delivery.Certified Lamaze Educators in a certified hospital play an important role in helping pregnant women make informed decisions about their pregnancy care and delivery. Lamaze classes are designed to provide expectant mothers with the knowledge and skills they need to have a safe and healthy pregnancy, labor, and delivery. Through these classes, mothers learn about the different stages of labor, relaxation techniques for pain management during labor and delivery, breathing exercises for comfort during labor, positions for pushing during delivery, as well as other helpful information. By taking a certified Lamaze class before giving birth, expectant mothers can feel more confident in their ability to handle the physical demands of childbirth.
How to Prepare for Lamaze Classes Before Delivery
Preparing for Lamaze classes before delivery is an important part of prenatal care. Lamaze classes provide yoga and other exercises designed to help pregnant women stay fit, relaxed, and healthy throughout their pregnancy. It is important to prepare for these classes ahead of time in order to get the most out of them. This preparation includes researching the type of class that you would like to attend, finding a qualified instructor, and learning about the types of exercises that will be included in the class. Additionally, it is important to discuss any concerns or questions you may have with your doctor or midwife before attending a Lamaze class. By taking these steps ahead of time, you can ensure that you are well-prepared for your Lamaze classes and get the most out of them during your pregnancy.
4D Scan Services

Oct 09, 2023 | 4 comments Reference
What are the benefits of a 4D ultrasound?
A 4D scan is a type of ultrasound that uses 3D imaging technology to create a real-time image of your baby in the womb. It is also known as a 3D-4D sonogram, and it offers an incredibly detailed view of your baby's features, movements, and activities. With this scan, you can get an idea of what your baby looks like before they are born, including facial expressions and body movements. The 4D scan can also detect any potential birth defects or other health issues that may be present in the fetus. Additionally, it can provide information about the position of the placenta and umbilical cord. Overall, a 4D scan is a great way to get an early glimpse into your baby's development in utero!
What are the benefits of a 4D ultrasound?
A 4D ultrasound can provide parents-to-be with more information about their baby’s development, such as the length, size, and position of the fetus. Other benefits to having a 4D scan include being able to see your baby move in 3D and seeing your little one in real time on screen. In addition to offering parents an opportunity to bond before birth, this type of scan can also be used during labor as an accurate way for doctors to monitor the fetus’ development.
Understanding the Difference between 2D and 4D Scans
Ultrasound scans are used to diagnose medical conditions and monitor the development of a fetus during pregnancy. 2D ultrasound scans provide a two-dimensional image of the fetus while 3D and 4D scans provide three-dimensional images. The difference between 2D, 3D, and 4D scans lies in their resolution and the abilities they offer for doctors to diagnose certain conditions.
2D ultrasound scan is the most common type of scan used during pregnancy. It provides a flat image of the fetus which can be used to detect abnormalities or measure fetal growth. 3D ultrasound scans cost more than 2D but it gives more detailed images of the baby’s face, body, and internal organs which helps doctors diagnose certain conditions more accurately.
4D ultrasound scan is an advanced version of 3D which provides real-time images that can be used for monitoring fetal movement in detail.
Ultrasound scan uses sound waves and a transducer to produce echoes which are then received by a computer along with the image.
The ultrasound images are then displayed on a monitor. A small hand-held device called an ultrasound transducer is used to generate sound waves and transmit them through the body of the fetus, generating echoes that can be received by the machine along with an image. These echoes are translated into real-time pictures which can be interpreted by a doctorThe doctor will analyze the images for any abnormalities or changes in development so they can determine the health of the child and his or her chances for survival.
What is IUGR?
Intrauterine growth restriction is defined as a decrease in foetal growth from the established norm. This might include a decrease in head circumference, weight, or other measures. The problem is usually detected by measuring body length and head circumference of the fetus during the second trimester of pregnancy. Intrauterine growth restriction typically occurs when an individual's weight gain falls below what is considered normal for their height. If this happens every month, it can be seen as "normal" even though it may be outside the healthy range for that particular individual. The most common cause of IUGR is maternal diabetes, and an increased risk of fetal growth restriction exists with maternal diabetes, preeclampsia, renal disease, and other chronic diseases such as hepatitis. Another cause is placental insufficiency.
Understanding How Fetal Growth Restriction can Lead to Serious Complications-
It is important to diagnose FGR early in pregnancy as it can lead to serious complications. The size of the fetus can be monitored during antenatal care, and if there is any concern about FGR, further tests should be done to diagnose it. FGR can lead to premature birth and low birth weight, which can increase the risk of health problems for both mother and baby. It is, therefore, important for pregnant women to seek regular antenatal care so that any issues with fetal growth can be detected early on and managed appropriately.
How to Choose a Quality and Affordable 4D Scan Service Provider
Choosing the right 4D scan service provider can be a tricky task. With so many options out there, it's important to find one that offers quality scans at an affordable price. Fortunately, there are a few tips and tricks you can use to make sure you get the best 4D scanning services available. When selecting a 4D scan service provider, look for one that has experience in providing prenatal care clinic services. Also, make sure they offer 3-4-dimensional scans with the latest technology and equipment.
Additionally, check their customer reviews and ratings to ensure they have a good reputation in the industry. Finally, compare prices from different providers to find an affordable option that meets your needs and budget. When taking a 4D scan, it's important to do your research and find a provider that offers quality images at an affordable price. Using these tips and tricks will help you narrow down the options and make the best decision possible.
How to Reduce the Risks of a 4D Scan by Conducting Simple Maintenance and Avoiding Unnecessary Procedures?
During pregnancy, it is important to reduce the risks associated with a 4D scan by conducting regular maintenance and avoiding unnecessary procedures. A 4D scan is a type of ultrasound that provides detailed images of the baby's development in the womb. While this technology can be incredibly beneficial for expectant parents, it also comes with certain risks. By conducting simple maintenance and avoiding unnecessary procedures, you can reduce these risks and ensure your baby's safety during this important time.
Maintain your weight gain throughout pregnancy: Maintaining a healthy weight gain is one of the most important steps in reducing pregnancy risks. If you are struggling to meet your weight gain goals, talk to your doctor about talking with them about dietary changes and other possible solutions that can make it easier on you and the baby. Discuss what you should be eating each day, how much, and when in order to make sure that this process is going as smoothly as possible for both you and the baby.
Go for an ultrasound every six weeks: Getting your regular ultrasound is an easy way to monitor how your baby is developing. This will also give you peace of mind that everything is running smoothly and any problems you may be having, whether it be with the placenta or the baby, will be caught before they progress too far.
The third phase is postnatal care with a focus on providing physical support to breastfeeding mothers as well as emotional support to new mothers who are experiencing postpartum depression or other mental health challenges.
Discuss your anxiety with a doctor: Anxiety can make pregnancy and motherhood difficult for some women and while it can't always be prevented, a lot of doctors in the field believe that one reason for this anxiety stems from poor symptom recognition and poor communication between patients and their doctors. This means that there are many things you could be doing that you are not aware of, and once pinpointed, will make a big difference.
What are Different Types of Equipment Used in a 4D Scan?
4D scans are the latest developments in fetal imaging technology, allowing expecting parents to get a detailed view of their baby’s development. 4D scans use specialized equipment to capture three-dimensional images of the fetus in real time. This provides a more accurate picture of the baby’s size, shape, and movements than traditional 2D scans. To perform a 4D scan, medical professionals must use specific types of equipment such as ultrasound machines, fetal monitors, and 3-4-dimensional scanners. With this technology, parents can get an up close look at their unborn child and gain insight into their development before birth.
postnatal maternal care

Oct 09, 2023 | 10 comments Reference
Introduction: What is a Fetal Viability Scan and When Should it be Conducted?
A fetal viability scan is an important part of prenatal care and can provide valuable information about the health and development of an unborn baby. It is a type of ultrasound scan that is used to assess the health and well-being of a fetus, including its size, position, movements, heartbeat, and possible abnormalities. The scan should be conducted between 18-24 weeks into pregnancy to ensure that the fetus is developing normally. During this time frame, doctors can also check for any signs of complications or potential risks that may affect the baby’s growth or development. It is important for pregnant women to get regular fetal viability scans in order to monitor their baby’s progress and ensure its healthy growth.
Examples of findings on a fetal viability scan can include:
● A healthy baby with good heart rate and no abnormalities
● An underdeveloped fetus with an abnormal heart rate, some small abnormalities, or the presence of fluid in the abdomen
● The embryo is not developing properly and is at risk for miscarriage
● The embryo has a poor blood supply and is at risk for developing conditions like anemia, low birth weight and prematurity
● The fetus has died or the gestational sac has ruptured
FAQs-
What is a viability scan? A viability scan is a medical test that can be used to assess the health of the developing fetus in utero. It involves using ultrasound to determine if there are any signs that the baby may need emergency, or non-urgent, intervention. If an abnormality is found, it can cause an increase in fetal distress and it will be necessary for a more invasive procedure to be performed on the baby.
Can I do an early fetal viability scan at home? Yes, you can purchase a home pregnancy test kit and perform your own early fetal viability scans at home. These kits generally have a window where you can do a scan.
Understanding the Different Types of Foetal Viability Scans in India
Fetal viability scans are an important part of pregnancy care in India. These scans help to monitor the development of the fetus, identify any potential risks and ensure that the mother and baby remain healthy throughout the pregnancy. There are three different types of fetal viability scans available in India – first trimester viability scan, second trimester ultrasound scan and 3d/4d ultrasound scan. Each type of scan
.
What is Postnatal Maternity Care?
Postnatal maternity care is a formalized health plan that provides support, guidance, and education to new mothers after they give birth. It can include a variety of different services both during and after pregnancy including nutrition counseling, breastfeeding support, postpartum doula services, physical therapy, lactation consulting services and more..
All of these services impact the mother's ability to recover from childbirth and enter into motherhood successfully. There are many different types of postnatal hand-outs that can be provided during this time which include basics such as what breastfeeding means for the mother and her baby, why it's important for the mother to rest after childbirth, the importance of prenatal care and a more comprehensive guide to postnatal care.
Why is Postnatal Maternity Care Important?
Postnatal Maternity Care is a set of health services provided to women during the postpartum period, which is the period of time after childbirth. It includes physical and emotional care for both mother and baby. It is important for women to receive proper postnatal care in order to ensure that they are healthy and well-cared for after giving birth. Postnatal care also helps to reduce the risk of complications, such as infection or depression, that can arise during this time. Proper postnatal care should be provided by experienced maternal healthcare providers who are knowledgeable about the needs of mothers and babies during this period.
The first phase is antenatal care, which includes monitoring and prevention of complications during pregnancy such as high blood pressure or diabetes.
The second phase is throughout the duration of the labor and delivery process and includes assistance with breathing, delivering a baby, pain relief and lactation.
The third phase is postnatal care with a focus on providing physical support to breastfeeding mothers as well as emotional support to new mothers who are experiencing postpartum depression or other mental health challenges.
It can be a very calm and relaxing experience for both the mother and the newborn,
Types of Maternity Care Services & Benefits to Postpartum Mothers
Maternity care services are essential for pregnant women and postpartum mothers. Antenatal and postnatal care are two of the most important types of maternity care services available. These services provide medical advice, guidance, and support to pregnant women throughout their pregnancy and postpartum period. Additionally, breastfeeding support services can be beneficial for new mothers who are trying to establish a successful breastfeeding relationship with their baby.
Mental health therapy services for moms can also be helpful in managing the stress and anxiety that often accompanies motherhood. Finally, lactation consultants can provide valuable advice regarding breastfeeding techniques and other lactation-related topics. All of these types of maternity care services can help ensure that new mothers have the knowledge and resources they need to make informed decisions about their health during this important time in their lives.
Postpartum Self-Care Tips for New Mothers
Becoming a new mother is an exciting time, but it can also be overwhelming. Taking care of a newborn and adjusting to life with a baby can be physically and emotionally draining. It is important for new mothers to take time for themselves and practice self-care. With the right postpartum self-care tips, new mothers can make sure they are taking care of their own needs while also caring for their baby. Postpartum self-care tips involve recovery from childbirth exercises, diet recommendations for new mothers, and sleep tips for moms.
Recovery From Childbirth Exercises- After giving birth, new mothers should start exercising immediately. These exercises can help improve the body and prevent any future injuries. It is important for new mothers to work out during their recovery period because it helps with muscle memory and reduces the risk of injuring themselves or hurting the baby. Postpartum self-care tips include walking, swimming, dancing, and yoga. New mothers should avoid exercising on their back until they have progressed through an exercise program that includes core strengthening exercises such as planks or crunches. By following these postpartum self-care tips , new mothers can prevent future injuries and be ready to take on the great life of motherhood.
Sleep Tips for Moms- Moms and partners should aim to have at least six hours of uninterrupted sleep each night which should include three hours in the first phase (stage) of sleep, followed by one hour in the second and third stages before beginning again in the first stage with another three hours. Moms and partners should aim to have at least six hours of uninterrupted sleep each night which should include three hours in the first phase (stage) of sleep, followed by one hour in the second and third stages before beginning again in the first stage with another three hours.
The Importance of Regular Health Checkups for Women on International Women's Day

march 07, 2024 | 10 comments Credit
What is International Women's Day and Why is It Important to Schedule Regular Health Checkups?
International Women's Day is an important event that celebrates the social, economic, cultural and political achievements of women around the world. It is also a day to remind us of the importance of taking care of our health and scheduling regular health checkups. Regular health checkups are essential for women to monitor their overall health and detect any potential issues early on. This includes physical exams, gynecological exams, breast exams, mammograms and other tests as recommended by your doctor. By scheduling regular health checkups, women can take control of their own self-care and ensure that they are receiving the best possible healthcare available to them.
Reasons Why Every Woman Should Have Regular Health Checkups
Preventing potential health risks- Some health screenings can help to identify potential health risks that a woman might be subjected to. These screenings may include Pap tests and mammograms, which are common for women at the age of 30 and 40 years old, respectively. Women should also talk with their doctor about whether they should get screened for breast cancer as early as twenty-five years old in order to catch any abnormalities as soon as possible. If you want to increase your chances of detecting precancerous changes, you can also consider getting an annual pelvic exam or adding an HPV test into your regular routine .
Early detection of cancer- A woman might also want to consider having Pap tests and mammograms performed in order to detect any cancerous changes as early as possible. Early detection is important to better monitor the progression of a tumor, which can help reduce the risk and duration of symptoms. If you are over fifty years old, you should probably consider undergoing a colposcopy once every two years. Women with high-risk factors for cervical cancer like being African American or smoking should get tested for HPV annually from age eighteen upwards.
Preventing potential complications from sexually transmitted diseases- Women who are sexually active should be screened for sexually transmitted diseases, such as HPV, at least once every three years. This is important because some sexually transmitted diseases can cause serious complications if left untreated. When it comes to HIV, this means getting tested for the virus once a year; however, some women should consider getting tested for HIV every six months since there are different treatment guidelines for pre- and post-treatment status.
Reducing your risk of ovarian cancer- Ovarian cancer is one of the most lethal forms of cancer that women can experience; therefore early detection can help reduce your risk of developing it. It's important to remember that five times more ovarian cancers are fatal than they are curable. The best way to prevent ovarian cancer is by undergoing screening tests like a pelvic exam, transvaginal ultrasound in order to detect any changes in the reproductive organs.
How to Prepare Yourself Before Going to a Regular Health Checkup
Going for a regular health checkup is important for any woman. It helps to detect any potential health issues before they become serious and can be treated easily. But, before you go for your regular health checkup, it is important to prepare yourself. This includes knowing what tests you need to take, understanding the various women’s health care guidelines and being aware of the preventive health screenings that are available. By doing this, you can make sure that you get the most out of your regular health checkup and stay healthy. Know What Tests You Need to Take Ideally, you should go for a routine checkup every year to keep your health up and avoid any potential problems. Before scheduling this appointment, it is important that you know what tests need to be conducted.
Breast examination, cervical examination, uterine screening, nutritional status- test for anemia, any other deficiencies.
The Importance of Informing Women about Their Health
Women’s health is a crucial aspect of their overall wellbeing, yet many women are unaware of the importance of preventive health screenings and gynecological screening tests. Women need to be informed about the various health screening tests they should undergo in order to maintain their health and detect early signs of illnesses. It is essential that women learn about the various preventive health screenings available and how they can benefit from them.
This includes understanding the specific guidelines for women’s health care, such as when to get tested and what types of tests are recommended. With this knowledge, women can make more informed decisions about their own healthcare, leading to improved outcomes. Women often do not get the preventive health screenings they need, which increases the risk of health and life-threatening diseases. Women should also be examined every three years because of the risk of cervical cancer. It is also important for women to know the guidelines for women’s healthcare, such as gynecological screening tests and other preventive measures. With this knowledge, women can make informed decisions about their health and well-being.
How Regular Health Checkups Help Keep Women Healthy and Protected?
It is essential for women to understand the importance of these screenings and tests in order to stay healthy and prevent any potential illnesses or diseases from developing. Knowing what tests are available, how often they should be performed, and what symptoms to look out for will help ensure that women are taking care of their bodies in the best way possible.
● Women with increased body mass index (BMI) are also at a higher risk for experiencing cardiovascular disease, type 2 diabetes, high blood pressure and stroke. Women who have had prior breast cancer or other cancers are also at an increased risk of developing a second cancer later in life
● By attending regular checkups, women can be protected from potential risks associated with their lifestyle or genetic make-up
● Women who smoke and drink excessively are at a higher risk for heart disease, high blood pressure, stroke, lung cancer and other diseases. Women who have been exposed to second-hand smoke are also at a great risk of heart disease, high blood pressure, stroke and other cancers. There is also evidence that suggests women who have had multiple miscarriages or stillbirths may be put at an increased risk of developing osteoporosis later in life.
● Women also have a higher risk for breast cancer due to their increased exposure to the hormone estrogen. It is important that women do not ignore their health risks and make sure that they take care of themselves whether they are experiencing symptoms or not.
How To Safely Celebrate Holi as a Lactating Mother and Newborn Caregiver

march 23, 2024 | 10 comments Credit
What is Holi and Why is it So Special for New Mothers?
Holi is a Hindu festival of colors celebrated in India and other countries with large Hindu populations. It is a joyous celebration that marks the beginning of spring and the end of winter. Every year, people gather together to celebrate Holi with vibrant colors, music, dance and food. For new mothers, Holi is a special occasion as it marks the start of their journey into motherhood. It is an opportunity for them to bond with their families and friends in a festive atmosphere filled with joy and laughter.
Moreover, Holi has many customs and traditions associated with it that make it even more special for new mothers – from smearing each other's faces with bright colors to playing games like 'Dhulivandan' or 'Holi Khel'. to singing bhajans, Holi is a day to remember. The festival of Holi brings with it many new traditions and customs that mark the beginning of spring. Here are some reasons why busting into colors during Holi has become a celebration for all those who celebrate this occasion.
It is a day for bursting with joy: One traditional custom associated with the festival of Holi is smearing each other's faces and bodies with bright colors. The excitement of breaking out into colors during the event provides an immense sense of joy, making it one to remember. Moreover, new mothers get to remember the joy of their new baby's birth by celebrating this event. The festival is also celebrated with a special game called 'Dhulivandan'. The way to play the game is to smother your opponent in brightly-colored powder while they cover your face and body in the same color of powder. This takes place until one person's body is completely covered in colors, earning them a spot as winner!
Tips to Celebrate Holi Safely while Breastfeeding & Caring for a Newborn
From choosing natural colors to wearing protective clothing, these practical advice on how to make sure that your baby is safe and secure during the festivities. So read on to learn more about how to make the most of this special occasion with your little one!
● Keep Your Baby's Temperature Normal Babies and children often get congested, especially when they are exposed to too much pollen, which may cause wheezing or a fever. During the festival of holi, a lot of flowers are used for decoration and playing, as it is also the spring season, pollen allergies are common. The best way to prevent such complications is by keeping your child's temperature normal throughout the Holi season.
This can be accomplished by ensuring that your baby stays indoors whenever possible and doesn't go outside without some sort of protection (a mask, a kimono/kurta/uniform, etc.) A common misconception regarding Holi is that it will help babies improve their immunity system. However, this is not true. The best way to prevent any allergies or respiratory complications is by ensuring that your baby is healthy and by keeping the temperature normal.
● Keep Your Baby Safe and Comfortable. Babies should be kept safe and comfortable during Holi, especially in case of accidental contact with watercolor powder or oil paints, which may lead to choking. To ensure this, babies should always have a soft blanket at their disposal that they can use to cover their face in case of any mishaps. As a precautionary measure, children should also be supervised while they play with any chemicals/paints or substances.
● Enjoying Holi with your babies should be allowed. This could be done by making a special room for your baby with watercolor paints, paper cutouts and children's books for them to enjoy and keep them company. You can also let your baby dance around the house to the music during this fun time!
● Stay Hydrated- The best way of staying hydrated is by drinking water throughout the day in moderation along with fruits (especially watermelon) and vegetables like cucumbers or pears that are high-water content fruits that can provide you with much needed hydration. It is unnecessary to restrict your and your baby's fluid intake, but rather the best way to ensure that they do not get dehydrated is by being frequently hydrated.
● Avoid Food and Beverages- The main reason for babies developing infantile seizures is due to their immature nervous or brain networks that don't help prevent the absorption of alcohol or other toxins in the body. As a precautionary measure, avoid food and beverages that might cause your baby to have seizures. As a lactating mother, one must take care of their dietary consumption. Examples are alcoholic drinks, cannabinoids containing sweets as well as frequent intake of caffeinated beverages like coffee and tea
Essential Items to Have on Hand When Celebrating Holi with an Infant
Holi is a fun and festive holiday, but it can be a bit tricky when you’re celebrating with an infant. To make sure your little one has a safe and enjoyable time, it’s important to have the right items on hand. Diapers, rash cream, natural color for holi, lukewarm water and other infant care items are essential for keeping your baby happy during Holi celebrations. With these items in tow, you can ensure that your baby is comfortable and protected from any potential skin irritations or allergies.
An Important Gift for the Baby- A number of gifts are appropriate for a baby during Holi. A gift that can be enjoyed by both you and your infant is a new set of infant clothes. The right outfit will provide the baby with a sense of comfort and security. For infants, clothing should not be too tight or restrictive, so something light-weight is best to avoid any discomfort or rubbing. that may irritate the skin. What better way to celebrate Holi than with a new outfit that your loved one will enjoy wearing?
Another gift you might want to consider is a new toy or stuffed animal. Babies tend to be sensitive, so toys made of soft materials are ideal for this time of the year. If your baby receives such an item, he or she can focus on enjoying it without any concerns about what others might think about his or her behavior during celebrations.
What's On the Menu for Holi?
Many Indian households prepare traditional Holi delicacies to be enjoyed during this time of celebration. One example is the popular Indian sweet called gulab jamun, soaked in sugar syrup. Other popular Holi delicacies include deep-fried doughnuts called bhajiyas and savory snacks like samosa and kachori. Relish all these holi foods in moderation and make sure your toddlers can have some too. It is healthy for the mothers and infants to be consuming good food and enjoying their day.
Celebrate Holi Safely During Pregnancy: A Guide for Expectant Mothers

march 23, 2024 | 10 comments Credit
Introduction: What is Holi and How to Celebrate it Safely While Pregnant
Holi is a popular Hindu spring festival celebrated in India and Nepal. It is also known as the “Festival of Colors” or the “Festival of Love”, as it marks the beginning of spring and celebrates love, joy, and brotherhood. Celebrating Holi while pregnant can be a challenge due to the potential risks associated with it. This article will provide tips on how to celebrate Holi safely while pregnant, and discuss some of the precautions that need to be taken in order to enjoy this special occasion without putting your health or your unborn baby at risk.
What is Holi?
Holi is a Hindu religious festival. It falls on the day at the end of the monsoon season when Hindus celebrate and remember how, according to legend, Lord Krishna removed all darkness from across the land during one night and sprang forth springtime. The celebration takes place on a large scale in India with colorful powders that are thrown by participants as they playfully chase each other around with water guns or toddy wagons or just go outside and frolic in between houses. The festival is celebrated throughout North India during March or April. In Nepal it is often celebrated in December.
Holi, the festival of colors, is an important festival in India. Celebrating Holi during pregnancy can be a tricky affair. There are certain precautions and activities that should be taken into consideration to ensure a safe and enjoyable Holi for the mother-to-be.
Holi Activities for Expectant Mothers
Holi is a time for joy and celebration, and pregnant women should not be left out. With special activities tailored to their needs, expecting mothers can enjoy the festival of colors without any worries. From playing with natural colors to participating in traditional rituals, there are plenty of pregnancy-friendly activities that pregnant women can take part in on Holi. These activities not only allow them to partake in the festivities but also help them stay safe during this time. With proper guidance, expectant mothers can enjoy the festival of Holi while taking care of their health and well-being at the same time.
tips on how to celebrate Holi safely during pregnancy.
● Create safe holi colors for the mother-to-be If possible, it is recommended to avoid Holi colors that are neon shades and those containing strong colored dyes like red, orange and purple. Other alternatives include using a natural food coloring like beetroot powder or turmeric powder. If you have to use non-natural food colors, be sure to wash your hands well after applying them on the skin.
● Wear sunglasses, slippers and long sleeves If you are going to be doing any outdoor activities during Holi, it is recommended that you always wear a hat to protect your eyes from the intense light.
● Watch out for germs and other harmful substances During Holi, it is important to stay vigilant about germs and other harmful substances that can cause skin irritation and allergies.
● Babies should not be given any colored food or liquids. It is recommended to keep babies away from brightly-colored foods and drinks as they may affect their health adversely. Pregnant women should also avoid drinking these colors during this time period because they may impact the fetus in a negative way.
● Keep baby wipes, Neosporin, and anti-sensitivity cream on hand. It is important to have these items on hand in case your skin becomes irritated or you are experiencing a rash.
The Do's & Don'ts of Celebrating Holi While Pregnant
Don’t drink alcohol or consume drugs. Alcohol can lead to fetal alcohol syndrome, which can lead to mental retardation and other health problems. Drug use is also not safe, as addiction and side effects can impact the pregnant woman and her baby.
Don’t eat raw fruits or vegetables that have not been thoroughly washed first. Pregnant women should be cautious about eating food contaminated with fecal matter, parasites, bacteria, fungi, viruses or worms because these factors may transfer to the expectant mother's bloodstream if she consumes them via consumption of improperly washed produce .Stay hydrated and eat healthy foods such as fruits, vegetables, and whole grains. These foods have a low risk of being contaminated with harmful substances.
Do take a break during the day and rest when you can. Pregnant women should avoid engaging in strenuous activities that may cause dehydration or oxygen deficiency such as working out too hard or playing sports without adequate breaks to rest. These activities can lead to miscarriage or premature birth if pregnant women do not take care of their well-being during recreational events.Make sure you stay up-to-date on your tetanus shot and flu shots before the beginning of Holi celebrations so that you are protected against these diseases. If you are planning on traveling during this time, inform your doctor that you will be away from home so they can get a shot for you if needed.
What Foods Should You Avoid Eating During Holi?
Eating the wrong food can cause stomach upsets and other health issues. What Foods Should Be Avoided on Holi? The festival of colors and joy, Holi is celebrated all over India. During the festival, which is known as the Festival of Spring in Sanskrit, people throw colored powders on one another. As a result, colors are everywhere and there are no boundaries to whom this practice can be harmful to. However, it is important to remember that despite the colors being beautiful, it may also cause health problems for some people.
For pregnant women in particular who are more prone to complications from eating certain foods during their pregnancy time, it is important to avoid eating these foods on Holi. It is a tradition for people to celebrate the festival of colors and joy with a meal during Holi. However, it is important to remember that foods like red meat, drinks containing “bhang” (cannabinoids) are to be restricted. As these may be harmful for the mother.